Introduction
Digital dentistry has gained popularity and become a routine part of clinical practice, encompassing areas such as digital planning, guided surgery, and rehabilitation with fixed prostheses and implants. Intraoral scanners, which offer a three-dimensional preview of prostheses with equal or better accuracy than conventional techniques, have improved the patient experience and optimized clinical time for dentists.
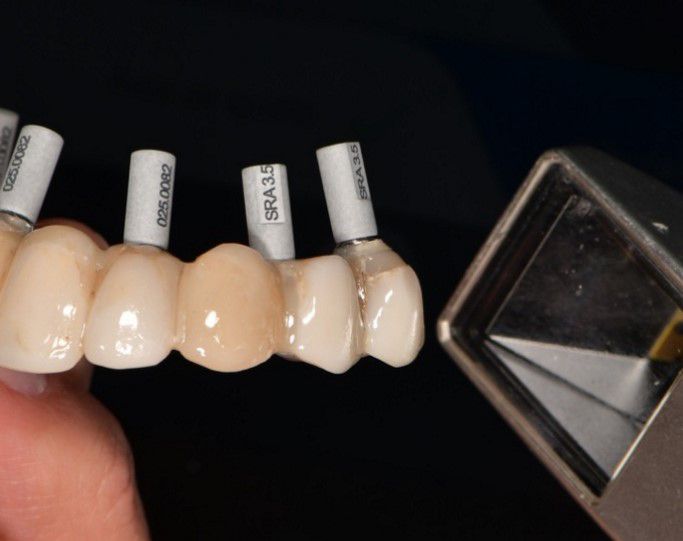
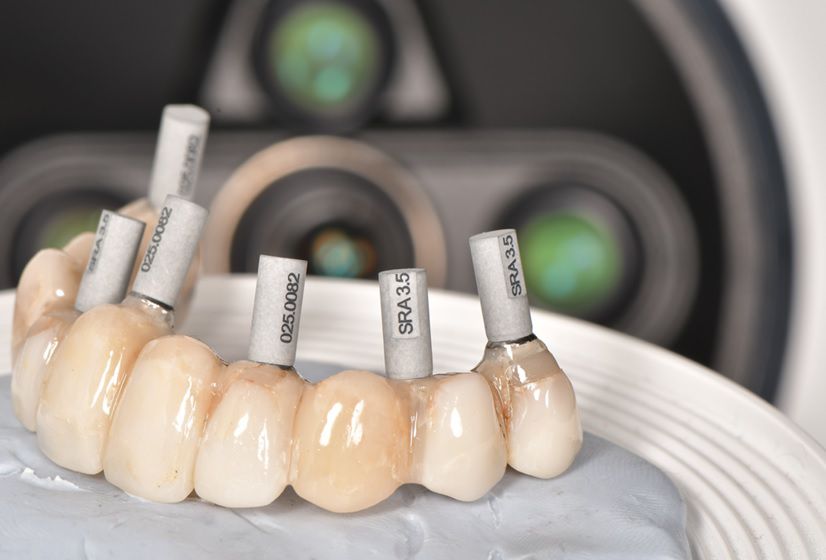
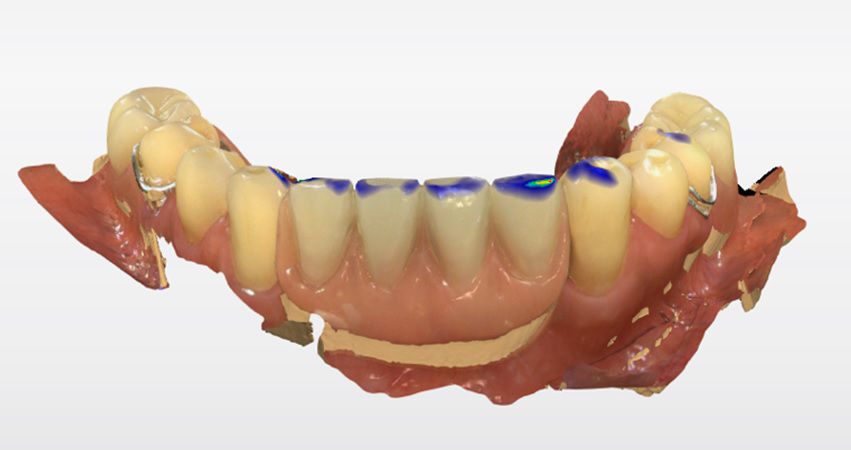
However, the digitization of completely edentulous ridges for implant-supported full-arch rehabilitation remains challenging, especially in the mandible, due to several technical and anatomical issues. To address these challenges, a solution known as the reverse scanbody has been developed. This innovative concept allows for accurate records of implant locations using extraoral scans of provisional prostheses.
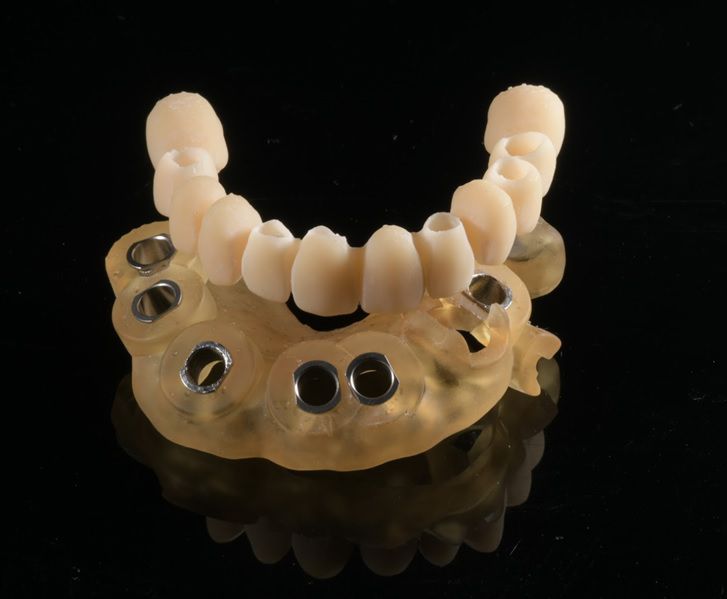
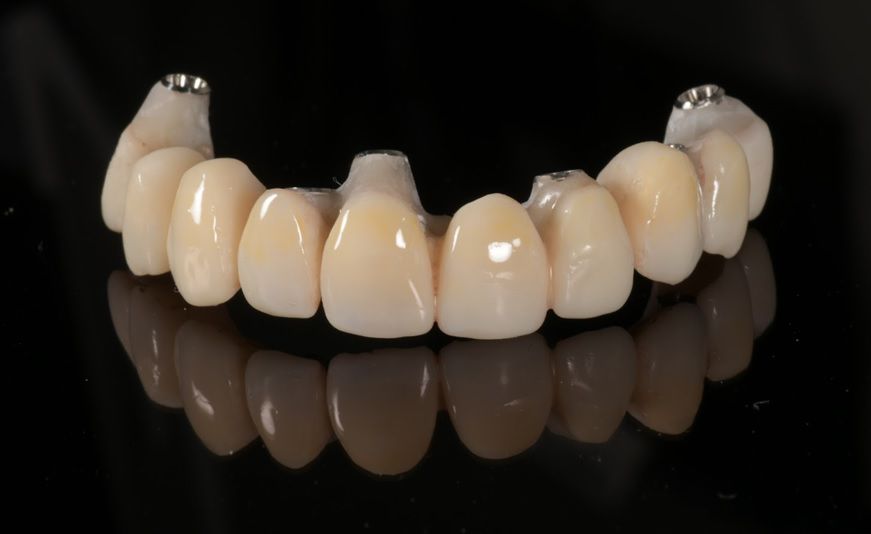
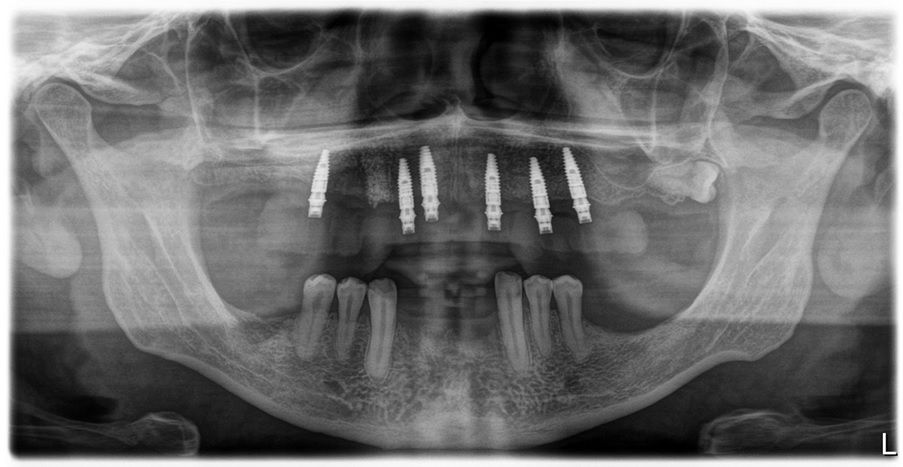
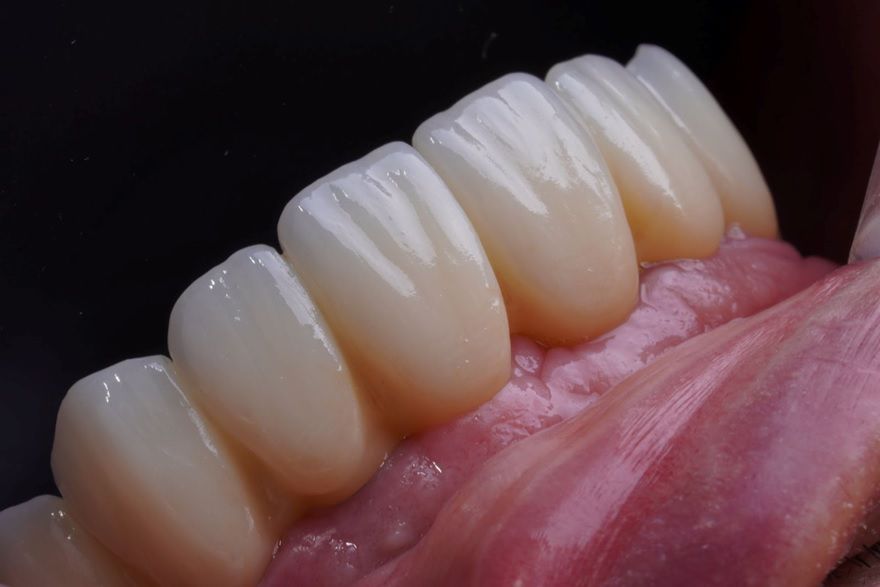
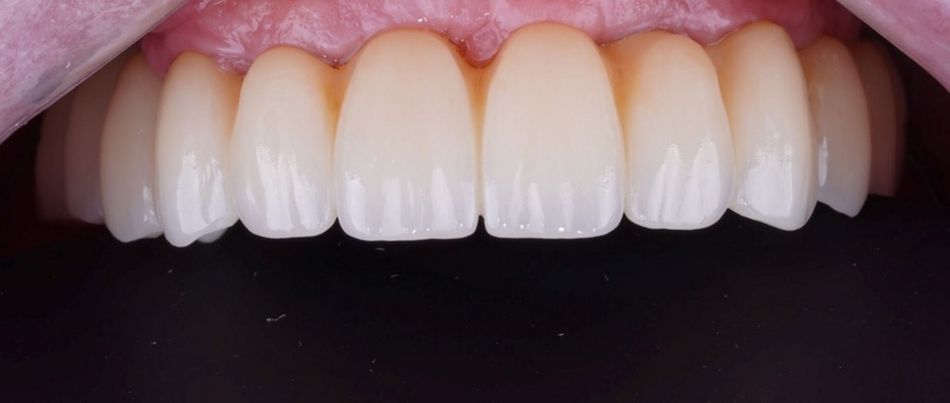
This case report highlights a full-mouth rehabilitation utilizing six Straumann® BLT ∅3.3 mm SLActive® Roxolid® implants and a digital workflow with Straumann® RevEX™ scan body. This comprehensive approach effectively addressed the patient’s functional requirements while exceeding esthetic expectations, resulting in a significant enhancement of confidence and overall quality of life.
Initial situation
A systemically healthy 42-year-old male non-smoker consulted for a definitive prosthetic solution.
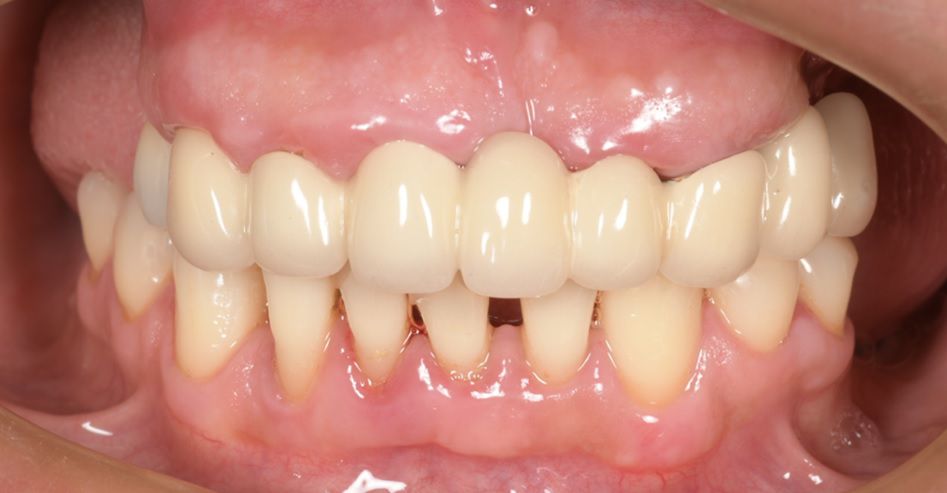
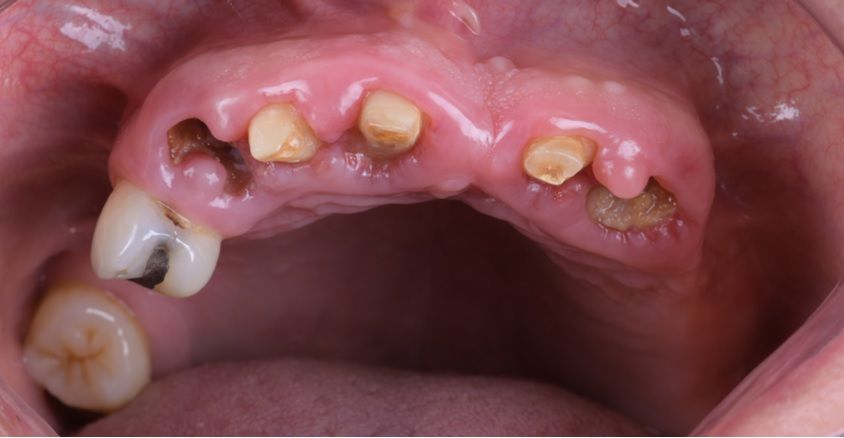
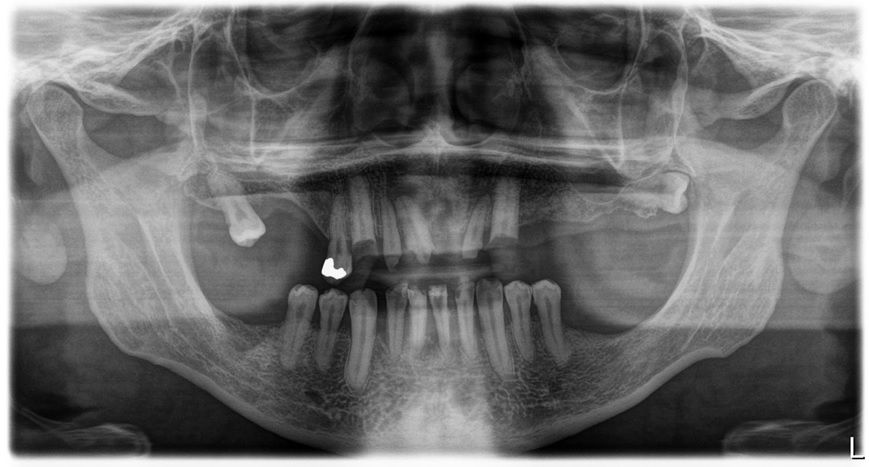
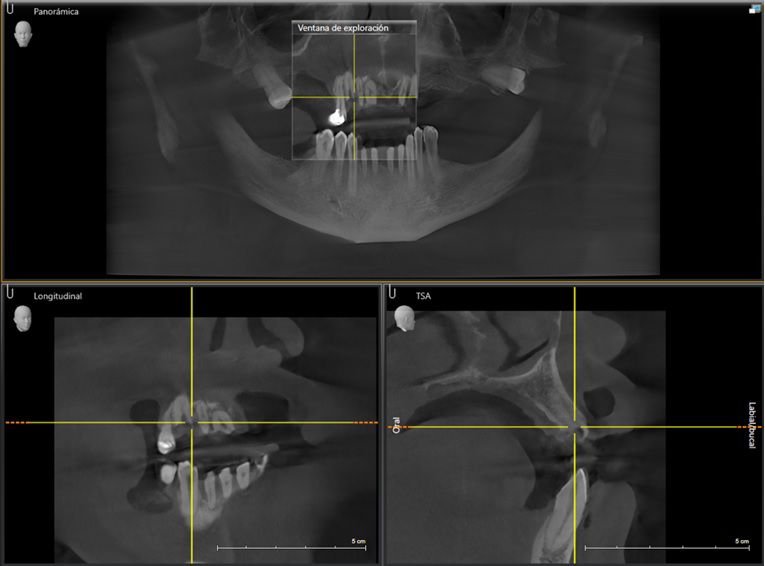
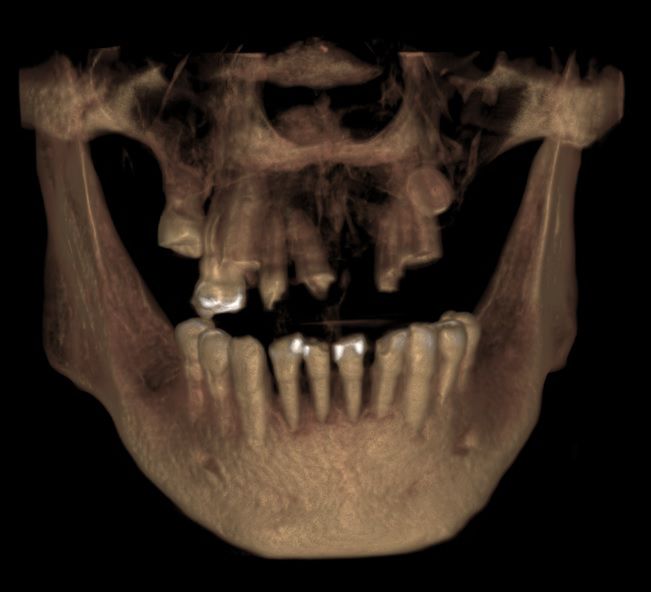
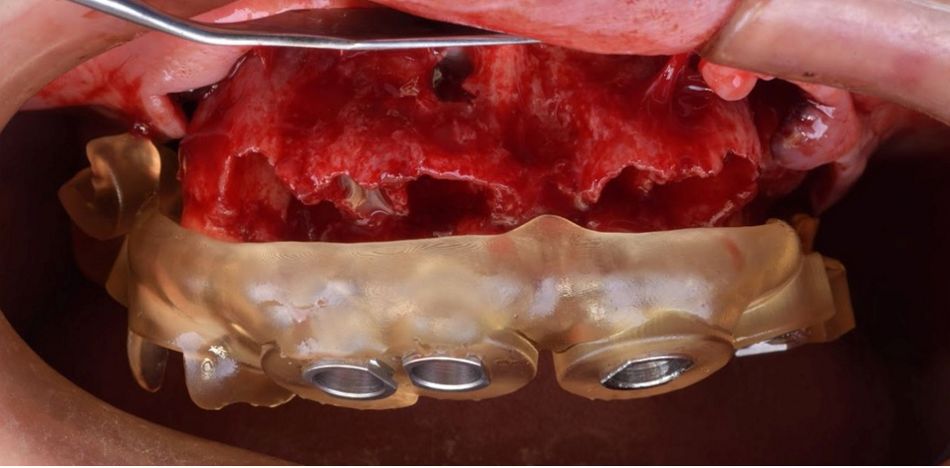
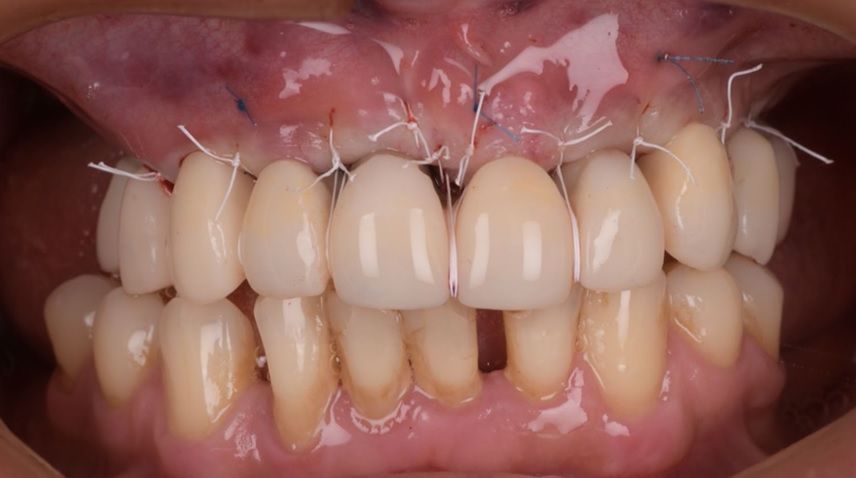
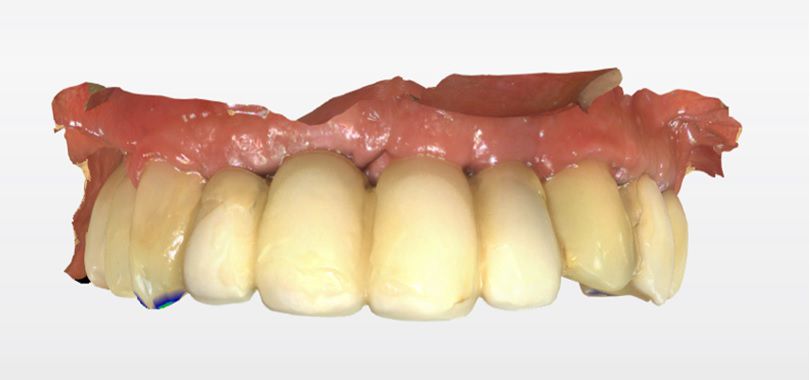
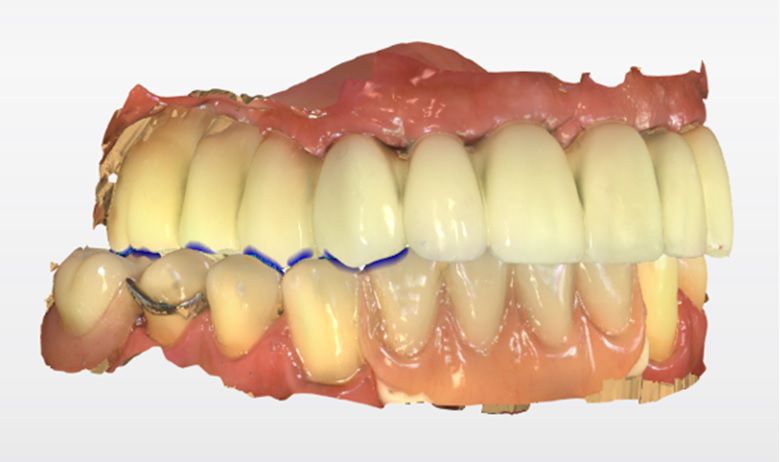
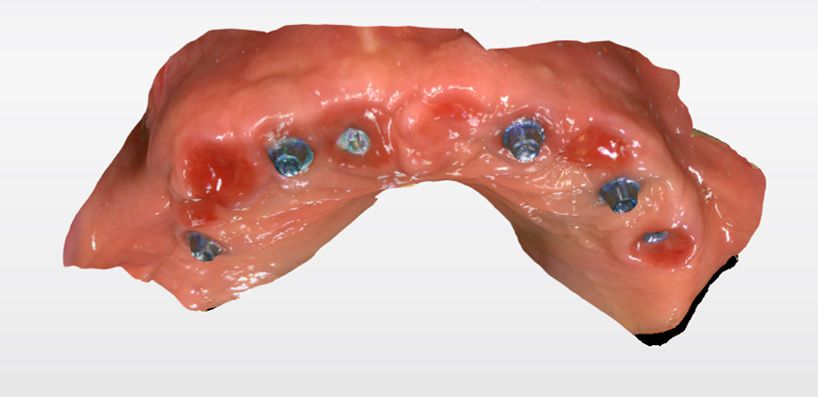
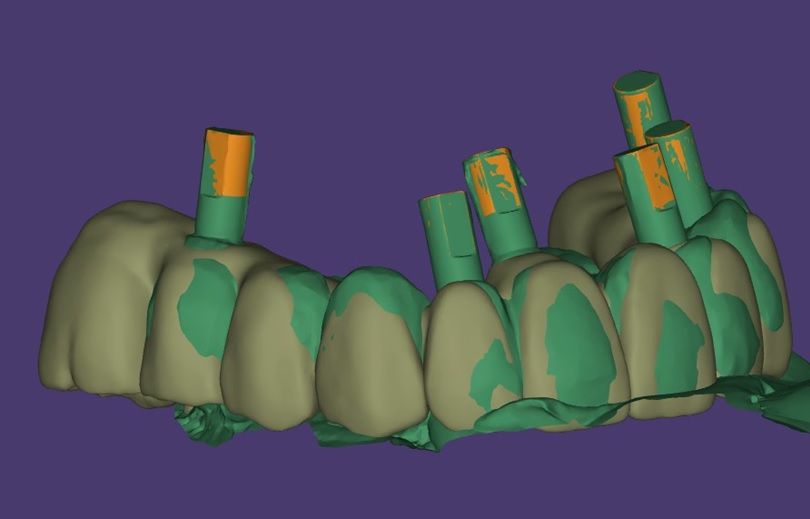
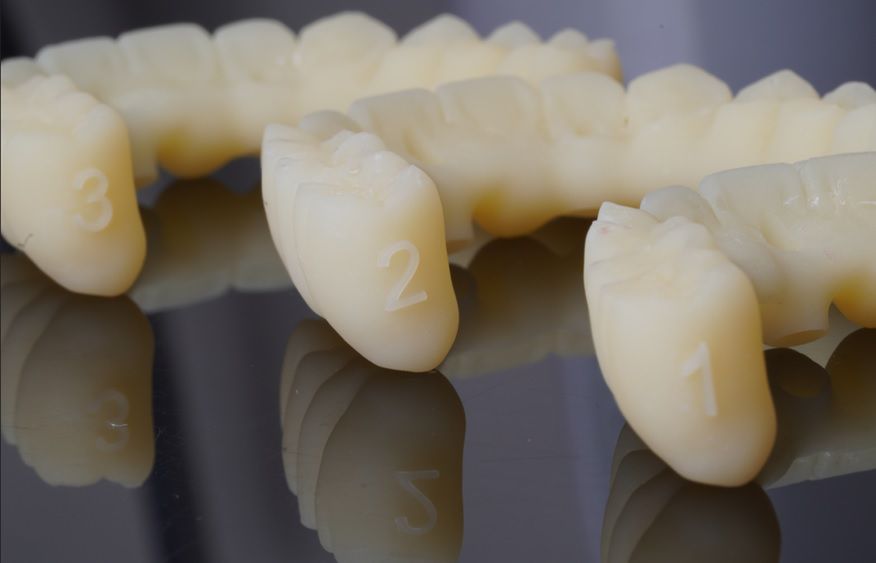
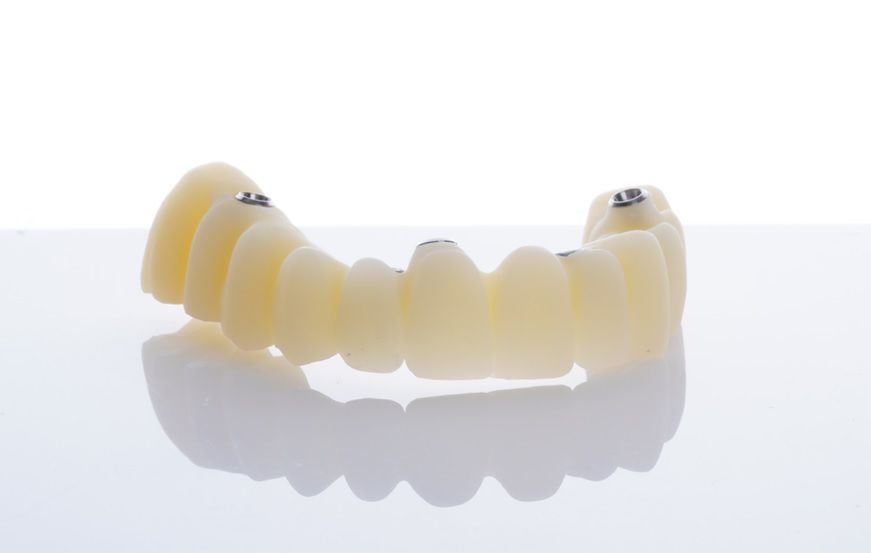
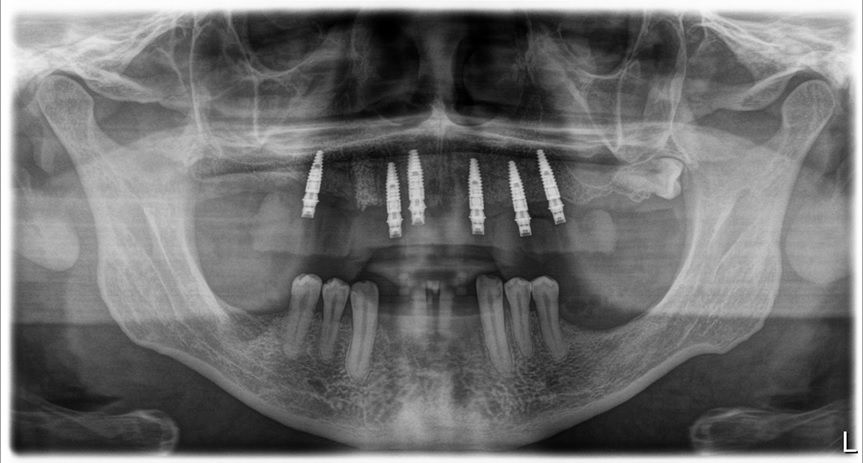
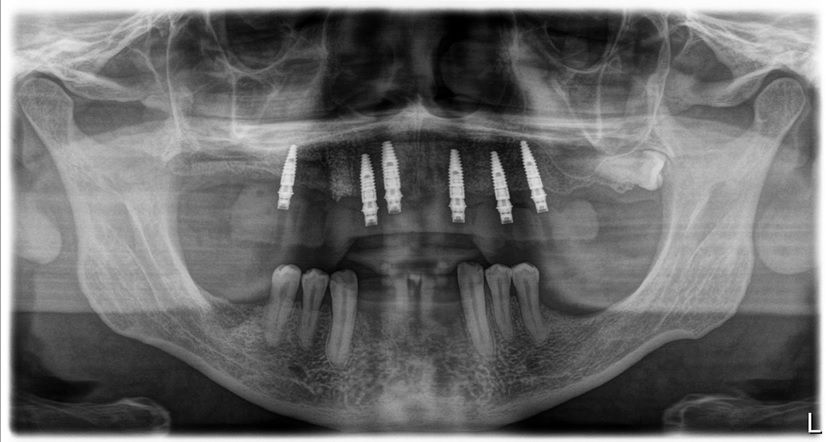
An intraoral clinical examination showed an upper plural fixed prosthesis spanning from #13 to #23, with coronal remnants lost due to secondary caries, an unfavorable prosthetic prognosis, and gingival inflammation associated with prosthetic misalignment. Additionally, there was significant horizontal and vertical bone resorption in sextants 1 and 3 (Figs. 1-5).
Treatment planning and surgical procedure